Ten days in hospital
I’m about to check out of Addenbrookes Hospital in Cambridge after a 10-day stay, 8 of them in isolation. The short story: I got a rash, and it took over my body. Below are some notes on what’s been going on, along with a few images. You can see the full set of images at http://bit.ly/terry-rash (you may need to register for Dropbox).
April 29 – May 5: The LCHF diet begins
 Just back from a week in New York, I decided to start a low carb, high fat (LCHF) diet. I’ve put on about a kilo of weight a year over the last 9 years and eating less carbs seemed like it might be a good way to start burning some of my excess fat. In 2012 I’d done some reading about LCHF diets but hadn’t tried it (check out this video if you’re curious). In NY I’d been feeling too physically large, which prompted me to give it a go. After almost 50 years of living on cereal, bread, pasta, rice and potatoes, though, I wasn’t sure I’d be able to do it.
Just back from a week in New York, I decided to start a low carb, high fat (LCHF) diet. I’ve put on about a kilo of weight a year over the last 9 years and eating less carbs seemed like it might be a good way to start burning some of my excess fat. In 2012 I’d done some reading about LCHF diets but hadn’t tried it (check out this video if you’re curious). In NY I’d been feeling too physically large, which prompted me to give it a go. After almost 50 years of living on cereal, bread, pasta, rice and potatoes, though, I wasn’t sure I’d be able to do it.
But it was suprisingly easy. I’d cook myself some bacon and eggs for lunch, along with a big salad, maybe a fried vegetable, nuts and dried beans for snacks, etc. Within a few days I was clearly in ketosis. I wasn’t getting hungry at all because my body had switched to burning my fat, and there was still plenty of that to consume. After 4 days I was down 3kg (from 78 to 75), or about 6.5 pounds. I felt like I was eating more healthily than ever.
Monday May 6: The rash appears
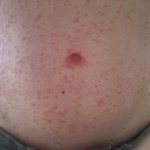
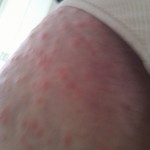
On the morning on Monday May 6, I awoke with a small itchy rash on my sternum, just small red separated dots, probably about 20 of them. I didn’t think too much of it.
Tuesday/Wednesday May 7/8: Initial spread
The rash grew across part of my chest and down my stomach. On the night of May 8th I slept on a fold-out bed downstairs so as not to bug Ana through the night. The rash was extremely itchy, but I knew I must not scratch it. I lay in bed wishing there were manacles by my sides to hold my arms down.
I had began searching around on the web for LCHF rash connections and found there were many hundreds of people blogging and commenting on forums about their rashes. But I couldn’t find anything that looked like reliable scientific opinion on what was happening to those people. Most of them had small rashes and many were able to stop the rash simply by reintroducing carbs. I added some carbs back to my diet, but there was no change. Almost all the comments online were reassuring, saying it was normal, that (unspecified) “toxins” were leaving my cells and exiting through the skin, etc. As so many people had similar problems, and they seemed to just go away after a while, I wasn’t too worried, just very itchy.
Thursday May 9
I had to take Findus to a doctor appointment after he got back from school. While there I showed part of my stomach to the doctor. She immediately said it was an allergic reaction. We didn’t discuss it further. I’ve never been allergic to any food, and hadn’t been eating anything new – just different amounts of foods I’d always eaten, and very few carbs. The doctor said she highly doubted the rash could be due to the diet change. She suggested I pick up some calamine lotion, hydrocortisone cream, and anti-allergy tablets to see if any of them helped.
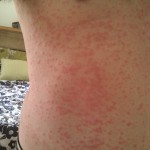
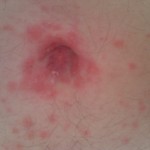
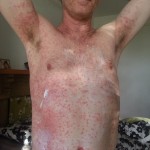
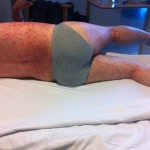
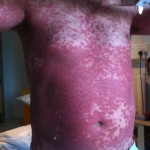
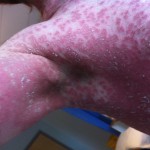
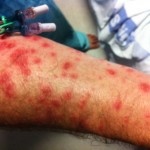
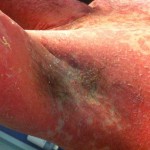
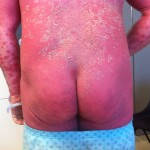
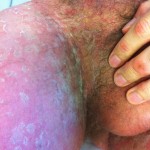
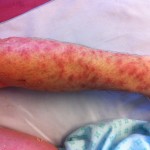
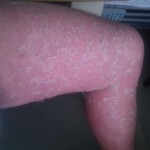
By this time, the fourth day, the rash had spread across under my armpits and slightly down my upper inner arms. It was all across my stomach, and my belly button was all rash (see image below). It had begun to descend onto my upper thighs. It was on my lower legs, just above my ankles, and on the back of my calves. My lower back was covered with it. Did I mention that it was itchy as hell?
Friday May 10
I went into Cambridge to meet people I’m doing some part-time research with (on virus detection and discovery, ironically). I was uncomfortable the whole time and spent much of the several hour meeting standing up. Sitting down was causing uncomfortable rubbing pressure on my pants line.
Late that night, Ana convinced me to call the emergency medical line. I didn’t feel it was warranted, but I admit I was worried. Plus, it was Friday night, the local surgery would be closed until Monday, and it was abundantly clear that if this thing didn’t stop spreading it was going to be really bad by then. A woman took my details, listened to the description, and decided to have the medical team call me. They did, and at 11:30pm I was given a midnight appointment at the Chesterton Medical Centre in Cambridge.
The doctor who saw me listened to my story and said I was having an allergic reaction. He put a bunch (8?) of triangular pink steroid tablets into a cup of water and got me to drink it. He wrote me a prescription for more. While talking to him I noticed an unusual slight twinge in my left eye, but didn’t think to say anything.
That night, the rash began to ooze. I noticed when turning over in bed that the sheets seemed to be wet. At first I thought I must be sweating a tiny bit without noticing it. After a while I realized the liquid was coming out of my body in tiny slippery beads of rash pus. Wet areas appeared on the sheets corresponding to my back, stomach, sides, thighs, etc. Very unpleasant. I didn’t sleep well, and not for the last time.
Saturday May 11
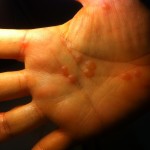
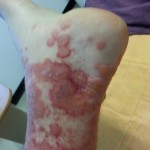
The rash has again spread and become denser. I filled the prescription and went into Cambridge with Sofia to meet Ana and the boys. Back home I took my first steroid dose. My right eye had begun to twinge too. Liquid-filled blisters were beginning to appear on the palms of my hands and on my fingers.
Sunday May 12
After another unpleasant night and more rash spreading, I called the emergency medical people again and got an immediate appointment at the Chesterton Medical Centre. I didn’t take calling for help lightly, but I was constantly uncomfortable and the steroids didn’t seem to have helped at all. The opinion this time was chickenpox. The doctor examined my eye but found no lesions on the cornea. So I went off the steroids and onto aciclovir tablets and aciclovir eye ointment. I was told to go to the Over Surgery on Monday to get a blood test for detection of chickenpox antibodies to confirm the dignosis. I mailed my parents to see if they could remember if I’d had chickenpox already. It seemed very likely that I must have, given that I did not get it when our 3 kids did.
Monday May 13: In isolation at Addenbrookes
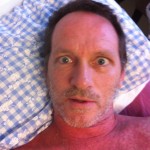
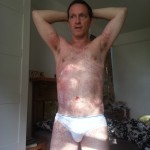
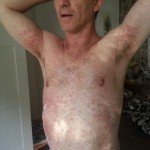
I’m not saying much about the physical side of things. The rash itself was mainly itchy. But my upper body had become extremely sensitive, and I could hardly bear for things to touch it. The sensitivity had been making me tense for some days, so I was not physically relaxed – far from it. My breathing wasn’t natural and even: I’d take in a breath and hold it a little to avoid breathing out and moving my body. Looking in the mirror at my whole body was quite shocking. Given the speed of the spread of rash and the discomfort level, it was clear that in a couple of days things would be really serious.
I called the Over Surgery at 8:30am and got a 9am appointment to have a blood test. I packed a few things in a small bag because I had a feeling I might not be back for a while. As it turned out, I wouldn’t be back home for 10 days.
On arrival, they sent me to a small room where a nurse did the blood samples. She asked why I wanted the test and I told her. I lifted up my top to show her some of my stomach and she said “I’m calling a doctor”. When the doctor did not arrive after a few minutes, she called another. They both soon arrived, and both said the same thing: go straight to hospital.
It’s about a 25 minute drive to Addenbrookes hospital from Over. They tried calling Addenbrookes to speak to the dermatologist, but couldn’t get through. So the doctor wrote me a letter to help with admissions and told me to go to the Accident & Emergency section. I would have much preferred to go in an ambulance than to drive. I guess uncertainty about driving showed in my face or body. The doctor said they could call one, but I declined. I went out and folded myself uncomfortably into the car. I knew I could hold on and keep it together, but I also felt like I was on the edge of some kind of collapse due to sensory or stress overload. It’s hard to explain, but I didn’t feel well at all. I told myself to focus, to act normal, turned on the radio and off I headed.
At Addenbrookes I drove into the carpark. UK parking places are invariably narrow, and I wasn’t looking forward to trying to get into one. Turning my body or stretching to see were painful. Up and up I crawled in a line of cars looking for places, all the way to the 6th level before finding a spot. Then a short walk, feeling a bit geriatric, to A & E.
Inside, they screen all arrivals. I handed over my introduction letter, was given a summary form, and told to sit and wait to be registered. I looked at the summary form, which had the usual mundane information: name, address, etc. At the top, a description of the reason for the visit. Mine said “Rash. Cause?” I was soon called to the registration desk and the woman took more details, including next of kin, and asked if anyone knew I was there. She was telling me I’d need to go sit down again to wait, but I needed attention. I said: “I know ‘rash’ doesn’t sound like much of a problem, but I think I need help right away”. I showed her my stomach. She took one look and sent me back to the woman doing the input screening, and told me to tell her my story. I showed the screening woman my stomach, and that was it. I was out of the admissions area at high speed.
In a small room, they asked me a few questions. I was already in the medical system as “Doctor Jones”. I knew I now had to mention that I’d been doing some work in the Viroscience laboratory at the Erasmus Medical Centre (EMC) in Rotterdam a few weeks earlier. As I wrote to my father later that night in email:
If you ever want to get expedited at top speed through hospital admissions, being called DOCTOR JONES, having spent recent time in one of the world’s top viral labs, and having an unexplained full-on bright scarlet 90%-coverage body rash ain’t a bad combo!
They took me straight to a small isolation room. When they left me there I heard them hang something on the door on the outside – it sounded like they were barring it! Nurses and doctors began to come by to ask questions, take blood samples and nasal/oral swabs. I had a canula line put into the back of my left hand. My heart rate was 120 on admission. Resting it is 60 or less. A Scottish nurse asked to see my back and exclaimed “Oh, you poor, poor, gentleman!”. I had no idea what my back looked like. Bad, I guess. The questions were about recent travel, what I had been doing in Rotterdam, medication, health history. Chickenpox, excema, other illnesses, allergies, the diet change. Sexual practices, drugs, medication, travel, animal exposure, etc.
About 5 hours after arriving, I was admitted and told I wouldn’t be going home that night. After a chest x-ray, I was transferred to an isolation room in Ward L4. It was a ward full of older post-surgery patients, not one used for infectious disease patients. But they needed an isolation room, and that’s what was available. The room was huge, with a window and en suite bathroom. Just as I arrived, I ran into Ana and Derek in the ward looking for me. I was happy to be in hospital, being looked after instead at home looking at my body with mounting dread.
Derek took some photos and emailed them to medical and virology friends at EMC to get their opinions and to ask if anyone else at EMC had come down with a similar condition. The prevailing thinking, at least at Addenbrookes, was that I had chickenpox. The blisters on my palms seemed the strongest indicator. Rather few diseases cause blisters, apparently. My parents had mailed me back to say they couldn’t be sure whether I’d had them.
Tuesday May 14
The night was long and uncomfortable. I wont go into details of the discomfort (see below for some of that). It finally got light around 4:15am. I spent hours standing around in the room naked, sometimes with a blanket around my shoulders but held off my body. I’d lean against the wall to stretch my back, and listen to the clock tick. At some point I realized the rash had gotten into my scalp. I hope my face will continue to remain free from it.
I don’t remember much about the day. Blood samples, swabs, antibiotics going into my arm, more doctors and more questions. Ana and Derek visited again. Ana brought fruit and other supplies, including my Nexus 7. I had almost no comfortable positions that I could maintain for more than a handful of minutes, but lying on my back was fine. The Nexus 7 would become my point of contact with the outside world. The small screen, a case allowing it to stand propped up on my chest, some of my music on it, and connected via a wifi hotspot made by my phone – perfect. I couldn’t have used a laptop.
I met Dr Sterling (head of Dermatology) that day and was very impressed. I also had a swarm of 5 female dermatologists staring intently at my skin as I stood naked in front of them. I told them I wished I had a camera.
An old woman named Margaret has moved into the room next door. She’s confused and disoriented. Every 5 or 10 minutes she walks out of her room and announces “I’m going home”. The nurses tell her she needs to go back to her room, that she’s in hospital, that she can’t go home. “I’m not a child you know, I’m going home.”
Wednesday May 15
Margaret wanders silently into my room as I’m eating breakfast. I don’t turn around, thinking it is a nurse. Her voice comes from behind me: “wrong house.” I don’t say anything, and she leaves. Later in the day, I am taking a pee and the door to my bathroom is open. I hear someone come in and call out to tell them I’m in the loo. There’s no response. Then I hear a voice call “Margaret, you’re in the wrong room.” Margaret calls back to them “my sister is here, she’s in the toilet.” By the time I come out of the bathroom, Margaret is gone. Later I hear them telling her that she’s going home today: “I certainly am not!” she replies, telling the staff that her friends are coming here to visit her and that she has to leave the ward to find them. No, no, they reassure her, your friends are coming here, they’ll come here to where you are. “But why would they come here?” I feel sorry for them all. Poor Margaret, and the nurses who have to look after her constantly coming out to declare she’s leaving and needing to be shepherded around the ward.
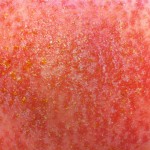
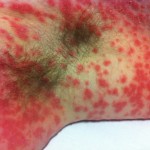
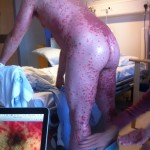
The coalesced parts of rash have gone a dark purple color. Meanwhile the rash has again spread and gotten denser everywhere. Blisters (at least 50 of them) are spreading on my palms and fingers. The VZV (Chickenpox) result came back negative, as did HSV (Herpes Simplex Virus).
With the negative chickenpox result, the case is suddenly more interesting and pressing. I met Dr Moore (head of Infectious Diseases) who comes to see me with Doctor Sterling. Dr Moore stared at me like a hawk, listened to everything very carefully, and then began asking questions. I liked her immediately, she seemed extremely smart and thorough. She suggested they move me to her ward tomorrow so I could be closer to the infectious disease people.
Tomorrow they’ll start throwing every test at me they can think of. Although the rash might be treatable with a steroid cream, the steroids suppress the immune system. So we need to figure out whether my body is busy fighting an actual disease before using steroids to try to settle what could otherwise be some kind of allergic reaction. The doctors here and at EMC start thinking of possibilities while the rest of us are digging for possible leads in Wikipedia, aided by Google Images.
What the hell have I got?
Thursday May 16: Skin pain like on that holiday trip to Mercury
The canula in my left hand has been hurting a lot when they pump in the antibiotics. So they’ve changed it, and put it into my right forearm. Unfortunately, the plastic dongle attachments hang down to the middle of my forearm where it is unbearably sensitive. Shit.
From a mail I sent to Ana & Derek later this night:
Skin pain like on that holiday trip to Mercury, the one where you forget to take any sunscreen.
During the day, Dr Sterling takes two skin biopsies taken from left forearm. Five stitches in them, in total. One of the samples will go into her -80C freezer and we’ll send it to EMC if necessary.
That night I have a pain in my trunk, back right, as I get up out of a chair. Derek is still there and I tell him. After 15 minutes of waiting for it to go away, we alert the staff. I’m almost unable to raise myself in bed to a sitting position so as to get up. One problem they’re watching out for is any kind of internal infection, so a pain in my right kidney region is a bit of a worry. I’m sent for a chest x-ray in wheelchair, and I have to wear a mask. More blood is taken and sent off for septic analysis.
Ahead of the transfer to Infectious Diseases, I have a shower. I have a 500ml container of anti-bacterial soap-like liquid and I’m supposed to wash my whole body. On my left forearm I have the two bandages (covering the stitches from the biopsies) that are not supposed to get wet, and sticking out the middle of my right forearm are two dangling plastic dongles attached to a canula with a tube going into my arm. So I’ve got one arm that can’t get wet and one that I can’t bend properly, and I’m supposed to have a shower and wash myself?
After somehow managing that, I begin putting liquid paraffin all over the rash. I.e., over my entire body. You know you have a real rash when they provide you with soothing ointments by the liter. Once I’m done, the rash feels better, but I am totally covered in shiny paraffin. I hang out naked for as long as I can and then put on the hospital pyjamas for the ward transfer.
I’m transferred at 8pm to Infectious Disease ward D10, and placed in isolation. There’s an air lock to get into the ward and a “Barrier Nursing” sign on my door. The room is about half the size of the one I’d just left, and cold. Derek goes to ask them if they can turn off the blower, but it’s part of the airflow set-up of the isolation ward. He gets me a small radiator to counter the cold and soon after that, around 9pm, they ask him to leave.
I now have about 9 hours to get through before I’ll see the morning staff. I lay in the dark with the Nexus 7 on my chest and sent a short mail to Russell:
This is utterly hellish. The last ward was a paradise. I half expect Derren to walk in. I should be tweeting it. It’s only 2am. I have to look at it as a survival course. I wish I could write more easily. This is left hand only for various reasons. I should make a list.
I didn’t want to expand on how horrible I felt, because it seemed extra words could only make it seem less horrible than it was. But I had nothing better to do, I was certainly not going to fall asleep, so I might as well write up a list of things that were collectively making this all so unpleasant. So from 2-3:20am, typing with the index finger of my left hand and lying on my back, I got it all down, big and small.
The main problem of course was that my skin was ridiculously sensitive and painful. To ease this, I was covered in paraffin, from toes to neck. The paraffin is all over the inside of the synthetic hospital pyjamas. It soaks, somewhat, into the rasping synthetic sheets of the bed and synthetic pillowcase. The bed blankets are heavy and synthetic, and they too don’t mix well with paraffin. Everything is saturated with paraffin. None of it dries out at all or becomes any less slippery or welcoming. Under the paraffin, concreted to my skin are thousands of small golden crystals of solidified rash pus (see image for May 13). They are very hard and scratchy, and are difficult to dissolve in the shower. It is like having large grains of sand in the paraffin between me and the bed. The air conditioner is constantly on, blowing cool air onto me, and making the sheets cold and dead to the touch.
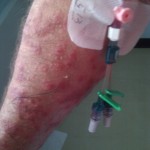
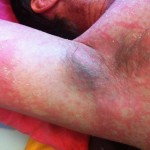
The skin pain is complimented by lots of things about my arms and hands that make it hard to do anything or be comfortable, apart from lying flat on my back. I have two cuts with stitches in them on my left forearm from the skin biopsies today. One of them has lost its dressing. I have a hospital name tag on my left wrist that is too loose. It will sound trivial, but it was extremely annoying. Hundreds of times, often using my mouth, I move it up and try to wedge it around my wrist, trying to keep it away from my forearm. The back of my left palm is bruised and sore from having a line in it for 3 days. The back of my right palm has been used about 10 times to draw blood. My right elbow crease area has the canula line in it, the tube going up into my vein above my elbow, making it uncomfortable to bend the arm. Two plastic dongle connectors hang from the line right to the exact middle of my ultra-sensitive forearm (see the image below). I need to find ways to position my arm so the plastic connectors are not resting on my forearm. Each time I move the arm, I try to avoid letting them touch me. The line hurts a little when the connectors dangle backwards out into the air, which happen if I raise the arm much (I am lying on my back, so raising the arm is a frequent need). The plastic bandage holding the line to my arm is half off, due to the paraffin, which makes it swing around more than it should.
There are about 60 blisters on my palms, between my fingers, and on the tops/bottoms of my fingers. Some are large, all are pressure sensitive. Closing my hands is awkward / sensitive due to this. Picking things up or, much harder, supporting my weight as I get up hurts the hands, for the same reason. I find it hard to bend down, let alone to reach the ground (skin pain) to pick anything up.
Lying on my back is fine, if I keep my arms angled out and clear of anything that could touch them or my underarms. But I have been lying down so much this past week, my back is very tired. Lying on my side is very uncomfortable due to arms, underarms, dongles, skin etc. I do it from time to time to relieve the back. I find a way to have both arms sticking out from my body, bent at the elbows, nothing touching anything, and I more-or-less hold the position and hope to drift off a little.
One thing I had been saving up and looking forward to as a midnight snack was a bowl of cereal with cold milk. After a couple of hours of lying in the bed, I decided it was time. I got up, feeling cold. I prepared the cereal and went to take the first delicious mouthful. Unbelievably, the milk had gone sour! I had to get warm again and the only place was the bed. But in the few minutes of preparing the cereal, I had left the sheets folded down and the air conditioner had blown on them. They were cold and saturated with paraffin. I forced myself back into the bed, pulled a blanket over myself, and tried to get warm.
At some point, I thought to myself “This is a survival course”. That everything that was going wrong, finishing with finding the milk sour and having to force myself into the wet sheets despite being freezing, was all part of a deliberate plan to break me. All part of a set of challenges I was being thrown and which I had to deal with. I mailed Russell, telling him I expected Derren Brown to walk into the room at any moment with a TV crew. The “survival course” perspective helped, and I began to smile (a little, inwardly). There was no way I was going to let this get the better of me. From then on, things have gotten better.
It was a horrible night. Probably the most uncomfortable of my life.
Friday May 17
My feet are now greatly swollen. Getting up from the bed is beginning to be painful. Negative test results come in on HIV and syphilis. During the day additional tests begin to come in.
Yesterday they weighed me: 81.6kg! I’ve somehow added 3.5kg in under 4 days. WTF?
Ana is worried I may have leukemia. It turns out she hasn’t slept for 3 days. The EMC guys have sent some worrying links, e.g., to things like Stevens Johnson disease. She brings me a ton of bedding: pillow cases, sheet, comforter cover, and a bunch of soft warm travel towels. That will make a huge difference.
Saturday May 18
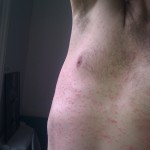
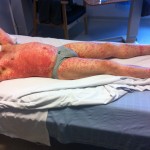
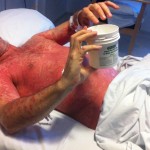
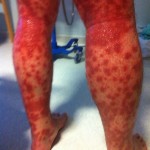
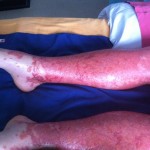
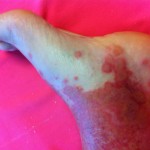
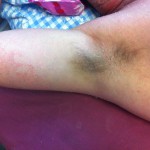
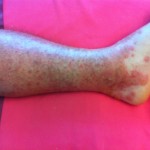
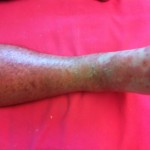
It’s hard to see that I used to have ankles. My lower legs have turned dark purple with the rash and are very swollen. Large ugly blisters have appeared on inside of my heels, around my ankles, and on my Archilles tendons, on both feet The right leg is worse, but it’s a close thing. The upper part of my body is looking quite a bit better – compare the earlier photo of my underarm.
Dr Sterling drops in. She thinks, given the negative infectious disease results, it’s time to try some steroid cream on just my stomach & chest. She examines my “tree stump” legs and takes a photo with her phone.
Dr Moore drops by too. She looks at my legs and tells me that due to some cellular protein level being low, water that would otherwise be bound and inside my cells is leaving them via osmosis and is basically sloshing around (I am paraphrasing) inside my system, causing the inflammation of my feet. She tells me I have to eat well, with as much protein as possible. She suggests protein shakes. I tell Derek, who lives on SPIRU-TEIN, and he brings me a can.
Ana comes by and is still terribly worried I may have leukemia. I call to get a doctor in some that she can hear why they don’t think so. Mok, who works with Dr Moore, comes by to help. He says he’ll ask the lab doing the biopsy to examine the white blood cells (my count is high) for any abnormal shape that might indicate leukemia. Mok comes by later to lance some of the blisters on my heels to collect their liquid for analysis.
That night I have a fever of 39C. But they’d given me paracetamol and codeine which keeps it in check. The codeine makes me feel totally weird. I am aware of the distant sensory roar from my skin as I lie with my arms touching the sheets. I can’t think clearly about anything. I see faces transform into mischievous devil caricatures, with goatees and horns. At about 3am I manage to collect myself and put the steroid cream onto my chest. The codeine weirdness goes on all night, until daylight. In the morning I find the canula in the bed next to me, the tube has been pulled out of my vein. I’ll not be trying the codeine again.
Sunday May 19
Sofia and Lucas visit with Ana. We eat Burger King that they bring and watch a movie. They look a bit shocked to see my upper body. I keep my pants on so as not to show my legs, which are much scarier at this point.
Getting into a standing position is now very painful. Pain shoots down my legs as the “sloshing” intra-cellular water pushes down through my legs. Then when my feet touch the ground, some of the water is forced back up my legs and pains shoot up to my inner thigh. Once I manage to stand, I have to take small shuffling painful steps for maybe a minute before things settle down and I can walk almost normally. If this keeps getting worse, getting out of bed is going to be a real problem.
I have very small new blisters on fingers. What’s going on, more blisters?
Monday May 20
The creep of additional rash redness on feet has continued overnight, and the rash is now between toes. Walking in flip flops affected. I realize I should have been putting the steroid cream onto my entire foot, not just the parts that visually (only) have the rash.
Ana and Derek bring delicious Indian food from Cambridge for lunch.
More infectious disease test results are coming in, all negative.
Tuesday May 21
Althea and Edward Parker visit. Rash creep on hands and feet has stopped. Liver structural damage sonogram test is negative. A stool enterovirus test comes back negative, ruling out Hand, Foot and Mouth Disease. I am declared officially non-infective, and get to go downstairs to coffee shop!
Derek drops by at night and we talk virus discovery and a presentation I’m due to give in Rotterdam next Monday. I’ve done no Fluidinfo work or anything else for a couple of weeks.
I am peeling pretty much everywhere. Each morning and evening I wash myself and apply steroid cream. In between I am constantly putting on a skin itchiness/excema moisturizer.
Wednesday May 22
I thought I’d be out today because the key liver test is now showing an improved result. But they want to keep me one more day to do another blood test for liver functionality. I’m tempted to let them take blood in the morning and then check out. If the result is bad, I can come back in.
At Costa coffee downstairs I begin to pull together the images (mine, Derek’s, Ana’s) from the weirdness of the last 9 days. I do some work on putting together the text for this blog post. Costa have a fast and free wifi network which you can use for 3 hours.
My legs are peeling so much. There are many large flakes of skin in the bed each time I get in or out. The peeling skin on my heels and back of my Archilles tendon is very thick. You wouldn’t think that skin could peel, but it can. The skin on your balls (if you have any) can peel too, I can confirm. It feels like I can rub cream into my feet forever and they still could use more. From shoulders down to feet it looks like I have a mild sunburn, skin either peeling or very dry.
Thursday May 23
I’m supposed to have a last blood test today, but they’ve not come as they usually do to take the sample. I’m totally packed up and ready to leave. It’s been 10 days.
Now I’ve had word, I’ll be out soon. They’re preparing the various ointments I’ll need at home. Blood just got taken again and the results will be back in about an hour. Next Wednesday I’ll come back in for another blood test.
Conclusions
There’s no strong conclusion as to what caused my rash. The doctors think the most likely explanation is that it was triggered by a virus, but they don’t know what. It could have been medication, but apart from some cough syrup and lozenges, I wasn’t on any. They say it’s not an allergic reaction, and that it’s not due to the diet change. If they’re right, I’m lucky, as it’s unlikely to re-occur.
The Addenbrookes people have been fantastic. Perhaps 100 people have looked after me over the last ten days. Many doctors, nurses, blood takers, food bringers, cleaners, wheelchair pushers, x-ray and sonograph operators, admin staff. They’re from all over: Poland, Hungary, Latvia, Zimbabwe, South Africa, Australia, Ghana, UK, India, Pakistan, Philipines, China. Everyone has been great. The nurses work 12 hour shifts. In a few hours I’ll be gone from here and someone else will be in this room, being taken care of just as expertly as I was, and the good people working here just keep going and going and going, making each patient feel special and cared for, for thousands of patients a year in this ward alone. I’ve had an unpleasant last 10 days, but compared to what some people go through on a much longer term basis, it has been nothing. I’m lucky, I’ll walk out in almost full health and soon be fully recovered.
And thanks so much to Ana and Derek, for coming by every day and taking so much care of me. That made a huge difference.
You can follow any responses to this entry through the RSS 2.0 feed. Both comments and pings are currently closed.




May 23rd, 2013 at 3:47 pm
OMG! Riveting reading. Not unlike NYT Diagnosis column, only those don’t worry me. Good time for a virtual hug.
May 31st, 2013 at 10:12 am
Oh man, that’s terrible. Glad you’re okay!
May 31st, 2013 at 10:20 am
Thanks Ross! :-)
September 16th, 2013 at 2:34 am
In 2000 I suffered from 90% eurythmedernic eczema and Staph. It was awful. dry skin, cracked weeping skin, lumpy spotty blistered skin,frogspawn spots on hands and feet, horrendously itchy and sore. Couldn’t stop scratching day or night skin tone altered to dark pink and red as if cooked in a big pan of boiling water. The only place free of skin problems was my face.
Had a temperature at the worst end of it and struggled to get a specialist appointment. I was eventally taken to a hospital and admitted. Felt I was going mad as self treatment, antihistamines and usual steroid cream didn’t work..
My treatment to begin with was test after test to see what it could possibly be as it didn’t look like normal eczema.
The specialist took a few skin biopsies but whilst waiting for results they began to treat my problem.
The first week in hospital consisted of Paracetamol and Codeine. Paracetamol for temperature and swelling, Codeine for pain. Potassium Pomangate and masses of Epaderm for bathing. After bathing 2 100 gram tubes of betnovate and 30 gram tubes of accylivir each day plus more epaderm. A 500 gram tub lasted 2 days. I was also prescribed a tranqilizer or antidepressant as this worked by slowing you down. I was also prescribed oral steroids at 40mg everyday for two weeks before the dose was reduced.
At night my skin seeped and stuck to my nightwear and bedding. I must have left a layer of crystals on the bedding each day when I woke.
Week two and three as above plus Zinc paste wet wraps and looking like an Egyptian mummy. Treatment shows signs of working in the middle of week three.
Week four as week 1 but lower strength paracetamol and codeine and lower strength tranqulizers and antidepressants.
Wraps continued with after care medications prescribed and continued oral steroids for a further two weeks.
.
10 months later and my skin had almost recovered, a bit opaque and very thin.
My father died in the October.
January 6th, 2014 at 10:13 am
Considering your nutritionally-deficient diet, it’s not surprising that your body developed this rash for a reason, for exercise, for homeostasis. Much like a muscle, your immune-system needs resistance training too.
April 2nd, 2014 at 5:01 pm
being one of the very fastest healing individuals known to several hospitals on the west coast and the US ARMY, i have quite the active Immune system, and adaptability is phenomenal… seeing this i recommend you try to do something to up that metabolism of yours, as it sounds like its creeping at a snails pace. Slow bodies resist less, lose weight slower, gain weight fast, and get sick faster. stimulants can be found abroad, mini markets etc… if you’re super slow then start with Cola, work your tolerance up to Baja Blast from Taco Bell, then touch RedBull, up to Rockstar/Monster, high protein diet, and keep active to help move along your new found high speed body, a high speed body loses weight fast, resists more illness better, gains weight slower… be warned though, instability of diet can lead to a brittle high speed, which has all the perks minus the strong antibodies, like seriously, you get coughed on and you catch the Tasmanian Devil as the Flu in your spine.
June 25th, 2014 at 3:34 pm
I seem to have this exact thing right now. The rash started on my torso and has spread down my arms and legs. It is on my neck but my face in not yet affected. I am at day 6, taking prednisolone 25mg (x2) and cephalexin 500mg (x4). My rash looks exactly like your photos in your Saturday May 11 photo. I am a 51 y/o female and the only change to my normal routine was the ingestion of cough syrup – Bonnington’s irish moss. I see in your blog that you also took cough syrup prior to the ‘rash’. Interesting! Though I am worried about the potential developement of the rash that you experienced.
June 25th, 2014 at 4:49 pm
Hi Jeanette. That looks bad…… there was no final conclusion in my case. The doctors considered the most likely diagnosis was DRESS (see http://en.wikipedia.org/wiki/DRESS_syndrome). I hope the above might be of some help. I guess you’ve been to a doctor? Feel free to mail me directly, I’m terry @ jon.es
June 26th, 2014 at 2:11 am
Hi Terry Thanks for your reply. Yes I have been to the doctor who ruled out measles, chicken pox, scabies or anything contagious. Although I did not see a dermatologist and had no conclusive blood, biopsy or fluid testing. They believe it to be an allergic reaction or viral and have prescribed steroids, antibiotics and anti-bacterial wash. My biggest concern is that I am holidaying in Bali in 10 days and the appearance of this rash is so shocking, i’ll look scary in bathers. Good news though, I woke this morning and the rash seems to be less red and angry (still incredibly itchy though) so maybe the steroids are having a calming affect. I’ll keep you informed.
January 20th, 2015 at 12:25 am
I don’t know why your pictures of this rash showed up while I was looking at bedding plants to put out next spring-but it did. It was painful to look at your pictures and even try to imagine the misery you were in. I think your attitude was incredible while going through all the medical tests and while being covered in such an angry skin rash. Even though this is way after the fact– I wanted you to know you have someone in Texas that admires you, thinks you handled a horrible situation far better than I would have and I hope all is well with you now!
May 29th, 2015 at 3:07 pm
im sorry that you had to go theough that but im glad you’re all better now. im curious have you fully recovered now? im really intrigued as i feel like i am experiencing what tou went through; rashes all over, oozing-making it challenging to sleep, swelling of the leg and general discomfort at the slightest touch. anyway im just wondering, how you got better because im a month into this dreadful experience. your feedback would greatly be appreciated. have a good day terry :)
May 29th, 2015 at 3:49 pm
Hi Adib. I’m sorry to hear you’re having a similar issue. I’m fully recovered, yes. But still in the dark as to what really happened. The steroid cream is what (apparently) got me on the path to recovery. BUT… the steroids are immunosuppressing, so if your immune system is actually fighting something then using a steroid cream is a really bad idea. They waited 4 or more days before using it on me, and then only a little to start out with, on my stomach / chest. That was after determining that they couldn’t find any sign of virus, bacterial infection, etc. So I can’t give any medical advice (and I’m not a medical doctor anyway). What does your doctor say? After I got out of hospital it was at least a month until my skin was back to normal – my lower legs were peeling and itchy for weeks.
September 19th, 2015 at 4:56 pm
These are caused by parasites, AKA worms. Every human has them and some worse then others. You need to do a parasite cleanse and get out in the sun to kill them.